Bovine Spongiform Encephalopathy
INTRODUCTION
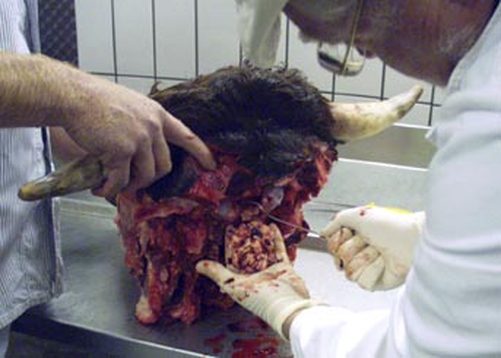
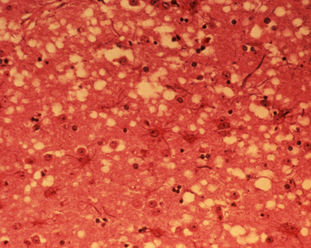
Bovine Spongiform Encephalopathy (BSE), commonly known as mad-cow disease, is a fatal neurodegenerative disease in cattle that causes a spongy degeneration in the brain and spinal cord. BSE has a long incubation period, about 30 months to 8 years, usually affecting adult cattle at a peak age onset of four to five years, all breeds being equally susceptible. In the United Kingdom, the country worst affected, more than 180,000 cattle have been infected and 4.4 million slaughtered during the eradication program.
The disease may be most easily transmitted to human beings by eating food contaminated with the brain, spinal cord or digestive tract of infected carcasses. However, it should also be noted that the infectious agent, although most highly concentrated in nervous tissue, can be found in virtually all tissues throughout the body, including blood. In humans, it is known as new variant Creutzfeldt–Jakob disease (vCJD or nvCJD), and by October 2009, it had killed 166 people in the United Kingdom, and 44 elsewhere.
Between 460,000 and 482,000 BSE-infected animals had entered the human food chain before controls on high-risk offal were introduced in 1989.
A British inquiry into BSE concluded that the epizootic was caused by cattle, who are normally herbivores, being fed the remains of other cattle in the form of meat and bone meal (MBM), which caused the infectious agent to spread. The cause of BSE may be from the contamination of MBM from sheep with scrapie that were processed in the same slaughterhouse. The epidemic was probably accelerated by the recycling of infected bovine tissues prior to the recognition of BSE. The origin of the disease itself remains unknown. The infectious agent is distinctive for the high temperatures at which it remains viable; this contributed to the spread of the disease in the United Kingdom, which had reduced the temperatures used during its rendering process. Another contributory factor was the feeding of infected protein supplements to very young calves.
The first reported case in North America was in December 1993 from Alberta, Canada.
Another case reported later in May 2003. The first known U.S. occurrence came in December of the same year though it was later confirmed that it was a cow of Canadian origin and imported to the U.S. Canada announced two additional cases of BSE from Alberta in early 2005. In June 2005 Dr. John Clifford, chief veterinary officer for the United States Department of Agriculture animal health inspection service, confirmed a fully domestic case of BSE in Texas. Dr. Clifford would not identify the ranch, calling that "privileged information". A new case of Mad Cow disease was recently found in a dairy cow on April 23, 2012 in California during a planned Agriculture Department surveillance program. United States health authorities were quick to point out that the animal was never a threat to the nation's food supply and claim that this is an atypical case of BSE caused by "just a random mutation that can happen every once in a great while in an animal".
Read more at WIKIPEDIA
Mad cow disease has hit the United States
Mad Cow confirmed in California
April 25, 2012 by RTAmerica
On Tuesday, a bovine in the state of California tested positive for mad cow disease.
The incident has caused health officials to address the issue and assure Americans that humans are not at risk. If a person was to consume meat that is infected with the disease, however, the victim would rapidly see a failure in mental health and movement ability.
Despite the dangers that could develop from the disease, two states have recently passed legislation that outlaws undercover investigation at factory farms. These "ag gag" laws could keep journalists from exposing the conditions that cause mad cow, yet now a third state is considering passing similar legislation.
Matt Rice from Mercy for Animals takes a closer look at the disease and how incidences of animal cruelty should be investigated.
Mad cow disease case in US was a 'one-off' caused by a mutation
The US Department of Agriculture says there should be no concern about safety of food supply after discovery of BSE Bovine Spongiform Encephalopathy (BSE), commonly known as mad-cow disease, is a fatal neurodegenerative disease in cattle that causes a spongy degeneration in the brain andspinal cord.
BSE has a long incubation period, about 30 months to 8 years, usually affecting adult cattle at a peak age onset of four to five years, all breeds being equally susceptible.[1]
In the United Kingdom, the country worst affected, more than 180,000 cattle have been infected and 4.4 million slaughtered during the eradication program [2] The disease may be most easily transmitted to human beings by eating food contaminated with the brain, spinal cord or digestive tract of infected carcasses
BSE has a long incubation period, about 30 months to 8 years, usually affecting adult cattle at a peak age onset of four to five years, all breeds being equally susceptible.[1]
In the United Kingdom, the country worst affected, more than 180,000 cattle have been infected and 4.4 million slaughtered during the eradication program [2] The disease may be most easily transmitted to human beings by eating food contaminated with the brain, spinal cord or digestive tract of infected carcasses
The US department of agriculture says there should be
no concern about food safety
April 26, 2012
The US department of agriculture says there should be no concern about food safety after the discovery of BSE in a US dairy herd. The disease apparently arose from a one-off mutation picked up during random surveillance at an abattoir in California.
The animal was tested as part of a regular inspection programme that examines tissue from 40,000 slaughtered cattle each year.
Dr John Clifford, the department’s chief veterinary officer, said the investigation was continuing, but added “there should be no concern . . . about the safety of our food supply.”
Despite this, two of South Korea’s largest importers of US beef halted sales. BSE in the food chain has been linked to cases in humans of variant Creutzfeldt-Jakob disease.
Source
The basics of Mad Cow Disease
April 27, 2012
Mad cow disease has hit the U.S. and questions about this mysterious disease abound. Here's what you need to know about mad cow disease.
What Is Mad Cow Disease?
Mad cow disease, or bovine spongiform encephalopathy (BSE), is a transmissible, slowly progressive, degenerative, and fatal disease affecting the central nervous system of adult cattle. The U.S. Department of Agriculture (USDA) has tested hundreds of thousands of cattle for BSE.
Researchers believe that the infectious agent that causes mad cow disease is an abnormal version of a protein normally found on cell surfaces, called a prion. For reasons still unknown, this protein becomes altered and destroys nervous system tissue -- the brain and spinal cord.
Does Cooking Food Kill the Prion That Causes Mad Cow Disease?
Common methods to eliminate disease-causing organisms in food, like heat, do not affect prions. Also, prions only seem to live in nervous system tissue.
Does Mad Cow Disease Affect Humans?
A human version of mad cow disease called variant Creutzfeldt-Jakob disease (vCJD) is believed to be caused by eating beef products contaminated with central nervous system tissue, such as brain and spinal cord, from cattle infected with mad cow disease. For this reason, the USDA requires that all brain and spinal cord materials be removed from high-risk cattle -- older cattle, animals that are unable to walk, and any animal that shows any signs of a neurological problem. These cow products do not enter the U.S. food supply. The USDA believes this practice effectively safeguards U.S. public health from vCJD.
According to the CDC, no cases of vCJD have been identified in the U.S.
Having said that, it is important to clarify the differences between variant CJD and another form of the disease, referred to as classic or sporadic CJD. Classic CJD has no known cause and occurs each year at a rate of one to two cases per 1 million people throughout the world, including in the U.S. and countries where mad cow disease has never occurred. It is not linked to eating nerve tissue from mad cow disease-affected cattle -- both vegetarians and meat eaters have died from classic CJD. CJD most commonly affects people over 65 and is usually fatal within six months from onset of symptoms.
What Are the Symptoms of vCJD?
The disease can affect all age groups and is very hard to diagnose until it has nearly run its course. In the early stages of vCJD, people have symptoms related to the nervous system, like depression and loss of coordination. Later in the illness,dementia develops. But only in advanced stages of the disease can brain abnormalities be detected by MRI (magnetic resonance imaging). vCJD is fatal, usually within 13 months of the onset of symptoms.
Is it Possible to Get vCJD From Eating Food Purchased in the U.S.?
It is extremely unlikely that this would happen. To prevent mad cow disease from entering the country, since 1989 the federal government has prohibited the importation of certain types of live animals from countries where mad cow disease is known to exist. This ban includes meat products used in human, animal, and pet foods. In addition, prohibiting high-risk animals from entering the food supply and the removal of central nervous system tissue from the food supply helps assures that BSE is not a risk to consumers.
Can You Get vCJD From Drinking Milk From an Infected Cow?
Milk and milk products are not believed to pose any risk for transmitting mad cow disease to humans. Experiments have shown that milk from mad cow-infected cows has not caused infections.
What About Other Products Made From Cow By-Products?The FDA stops the importation of cosmetic and dietary supplement ingredients containing bovine materials from animals originating in the 33 countries where mad cow disease has been found or from animals at risk of being infected.
What Is the Current Risk of vCJD to Americans Traveling Abroad?
According to the CDC, the current risk of acquiring vCJD from any specific country appears to be extremely small. But that cannot be precisely determined because cattle products from one country might be distributed and consumed in others.
How Long Have Health Officials Been Concerned About Mad Dow Disease?
Mad cow disease has been of great concern since 1986, when it was first reported among cattle in the U.K. At its peak in January 1993, almost 1,000 new cases per week were identified. Concern about this disease grew significantly in 1996 when an association between mad cow disease and vCJD in humans was discovered.
What Other Countries Have Reported Cases of Mad Cow Disease?
The disease also has been confirmed in cattle born in Austria, Belgium, Czech Republic, Denmark, Finland, France, Germany, Italy, Ireland, Israel, Japan, Liechtenstein, Luxembourg, the Netherlands, Poland, Portugal, Slovakia, Slovenia, Spain, Switzerland, and the U.K.
Canada has also been added to the list of countries from which imports are restricted, although that ban has been lifted recently. Importation of minimal-risk meat products is now allowed from Canada.
Source
Mad Cow Disease and Humans
Brain disorder becomes deadly over time
The following is an article from 2006
Variant Creutzfeldt-Jakob disease (vCJD) is the "mad cow" disease that people contract when they are exposed to food contaminated with bovine spongiform encephalopathy (BSE). As of November 2006, 3 individuals with mad cow disease had been identified in the United States. The Centers for Disease Control and Prevention (CDC) monitors the incidence in the US of all types of Creutzfeldt-Jakob disease.As of November 2006 there were 200 individuals worldwide diagnosed with mad cow disease, including 164 people in the United Kingdom, 21 in France, 4 in the Republic of Ireland, the 3 in the US, 2 in the Netherlands, and 1 each in Canada, Italy, Japan, Portugal, Saudi Arabia, and Spain, according to the CDC. Of these individuals, most (170) had lived in the UK for over 6 months during the years 1980-1996; 20 others had lived in France during that time.
Disease has no cure
The public has good reason to be concerned about the transmission of BSE to humans. Variant Creutzfeldt-Jakob disease, like the other types ofCreutzfeldt-Jakob disease, is a brain disorder which becomes deadly over time. There is no cure.
Normally, Creutzfeldt-Jakob disease occurs in a person in one of three ways:
- About 10 to 15 percent of cases are inherited, resulting from a gene mutation.
- Most cases seem to appear sporadically, in someone who has no family history of the disease.
- A small percentage of cases occur through infection, by contact with infected brain tissue. There are documented cases that occurred as an unintended consequence of a medical procedure.
Creutzfeldt-Jakob disease is not contagious in normal ways, like sneezing or coughing--there are no known cases of spouses or family members of an infected person contracting the disease.
Contaminated beef products implicated
Variant Creutzfeldt-Jakob disease seems to have been caused by people eating contaminated beef products in Europe. The same disease, when it occurs in sheep, is called "scrapie." It is believed that scrapie-infected sheep products were used in cattle feed, and thus the cattle became infected.
Scientists have found that what causes BSE, scrapie, and the Creutzfeldt-Jakob diseases is not a virus or bacteria as in other diseases, but a protein agent called a prion. The prion transforms normal proteins into infectious, deadly ones.
Affects the brain
Since Creutzfeldt-Jakob disease affects the brain, the symptoms it produces are neurological. It may start out subtly with insomnia, depression, confusion, personality and behavioral changes, and problems with memory, coordination, and sight. As it progresses, the person rapidly develops dementia and involuntary, irregular jerking movements called myoclonus.
In the final stage of the disease, the patient loses all mental and physical functions, lapses into a coma, and eventually dies. The course of the disease usually takes one year. The disease generally affects people between the ages of 50 to 75 years. Variant Creutzfeldt-Jakob disease is called "variant" because it has affected people at a younger age, even teenagers (the ages have ranged from 18 to 53 years old).
Difficult to diagnose
There is not, as yet, a definitive medical test for diagnosing Creutzfeldt-Jakob disease. Since the disease is rare, some physicians might not even consider it as a diagnosis, and might mistake the symptoms for other brain disorders like Alzheimer's or Huntington disease. Scientists suggest that new, sophisticated laboratory testing will in the future be able to detect the prions in an infected person's blood or tissues.
Sources:
- Collins, S., A. Boyd, A. Fletcher, M. F. Gonzales, C. A. McLean, C. L. Masters. "Recent advances in the pre-mortem diagnosis of Creutzfeldt-Jakob disease." J Clin Neurosci 7(2000): 195-202.
- "vCJD (Variant Creutzfeldt-Jakob Disease)." NCIDOD. 29 Nov 2006. Centers for Disease Control and Prevention. 28 Dec 2006 <http://www.cdc.gov/ncidod/dvrd/vcjd/>. - Will, R., M. Zeidler, G. E. Steward, M. A. Macleod, J. W. Ironside, S. N. Cousens, J. Mackenzie, K. Estibeiro, A. J. Green, R. Knight. "Diagnosis of new variant Creutzfeldt-Jakob disease." Ann Neurol47(2000): 575-582.
- Wilson, K., C. Code, M. Ricketts. "Risk of acquiring Creutzfeldt-Jakob disease from blood transfusions: Systematic review of case-control studies." BMJ 321(2000): 17-19.
Source
Blood test helps diagnose deadly mad cow disease
January 16, 2012
A NEW blood test to identify the human form of mad cow disease is being developed by British scientists. Researchers have created the test for the deadly variant Creutzfeldt-Jakob disease (vCJD), which is being offered to British patients for the first time. Experts said the test represented a “significant step forward” in the fight against the disease as it will enable doctors to find out how many people are infected with vCJD. –TG
Neurologists across the country have been told by the NHS National Prion Clinic, part of the University College London Hospitals Trust, and the Medical Research Council’s Prion Unit that the new blood test is now available.
Until now the only way of confirming the diagnosis has been through tonsil biopsies or after the patient has died when brain samples can be taken. Prof John Collinge, who is leading the MRC team, told Channel Four News that the blood test was “extremely good news”.
“In principle, it may allow us to find how many people in the population are infected so we can target risk management strategies and ensure the safety of our blood supply,” he said. “It could also enable us to make an earlier diagnosis and as treatments become available it is going to be desperately important to get to patients early before there is extensive damage to the brain.”
Further testing will now occur to ascertain its realiability, which will involve examination of 5,000 anonymous samples supplied by the American Red Cross. Figures from the Health Protection Agency show there have been 176 cases of vCJD from since it was first detected in humans in 1995.
Variant Creutzfeldt-Jakob Disease is the human equivalent of Bovine Spongiform Encephalopathy (BSE), which affects cattle. Identified in the 1990s, the illness was traced to the consumption of beef products containing contaminated meat.
VCJD progressively causes the brain to become riddled with holes, leading to mental problems, loss of body function, and eventual death. There is no cure. The Department of Health’s working estimate is that 1 in 4,000 people - or about 15,000 individuals - are infected.
Source
A NEW blood test to identify the human form of mad cow disease is being developed by British scientists. Researchers have created the test for the deadly variant Creutzfeldt-Jakob disease (vCJD), which is being offered to British patients for the first time. Experts said the test represented a “significant step forward” in the fight against the disease as it will enable doctors to find out how many people are infected with vCJD. –TG
Neurologists across the country have been told by the NHS National Prion Clinic, part of the University College London Hospitals Trust, and the Medical Research Council’s Prion Unit that the new blood test is now available.
Until now the only way of confirming the diagnosis has been through tonsil biopsies or after the patient has died when brain samples can be taken. Prof John Collinge, who is leading the MRC team, told Channel Four News that the blood test was “extremely good news”.
“In principle, it may allow us to find how many people in the population are infected so we can target risk management strategies and ensure the safety of our blood supply,” he said. “It could also enable us to make an earlier diagnosis and as treatments become available it is going to be desperately important to get to patients early before there is extensive damage to the brain.”
Further testing will now occur to ascertain its realiability, which will involve examination of 5,000 anonymous samples supplied by the American Red Cross. Figures from the Health Protection Agency show there have been 176 cases of vCJD from since it was first detected in humans in 1995.
Variant Creutzfeldt-Jakob Disease is the human equivalent of Bovine Spongiform Encephalopathy (BSE), which affects cattle. Identified in the 1990s, the illness was traced to the consumption of beef products containing contaminated meat.
VCJD progressively causes the brain to become riddled with holes, leading to mental problems, loss of body function, and eventual death. There is no cure. The Department of Health’s working estimate is that 1 in 4,000 people - or about 15,000 individuals - are infected.
Source